As treatment for breast cancer continues to progress and improve, the focus for the healthcare community and patients is to address quality of life long-term. Lymphedema is one negative side effect of cancer treatment, which can affect someone lifelong. Breast cancer-related lymphedema affects 1 in 5 individuals following treatment for breast cancer.
There is significant importance in understanding what increases someone’s risk of getting lymphedema and what may lower the risk. It’s also crucial for both healthcare providers and patients to learn about what signs and symptoms to look for to detect lymphedema early and possibly be able to prevent it. Let’s talk about each of these.
Who is at Risk?
Individuals have between 20 and 40 lymph nodes in their armpit, also known as the axilla. Lymph nodes may be biopsied to evaluate and assess if cancer has spread outside the breast region. Typically, 1-5 lymph nodes are removed for a biopsy, which is called a sentinel lymph node biopsy (SLNB). If someone has a higher number of lymph nodes out for evaluation or to be removed due to cancer being found, this is called an axillary lymph node dissection (ALND). If someone has an SLNB, the risk of getting lymphedema is low, at about an 8% chance or less in a lifetime. Someone will have a higher risk of getting lymphedema if they have an ALND, which increases the risk to about 25%.
Additional Risk Factors
Radiation therapy to the chest and armpit area may also increase the risk of lymphedema because the radiation can cause radiation fibrosis. Radiation fibrosis is scar-tissue-like changes to the muscles, vessels, and other body tissues. If an individual had an SLNB combined with radiation, the risk of lymphedema is about 11%. If someone had an ALND combined with radiation, it increases the risk to about 30%.
Body mass index (BMI) or weight is another risk factor. If someone’s BMI is >30 or considered obese, this can cause an increase in the risk of developing lymphedema. You can find a BMI calculator HERE.
After having lymph nodes removed or radiation, lymphedema is considered a lifetime. However, lymphedema is most likely to occur and show up in the first 1-2 years of cancer treatment, so it’s essential to work with your medical team and monitor closely for any signs and symptoms.
Precautionary Risks
In the past, it was encouraged that those at risk for developing lymphedema should avoid lifestyle risks such as blood pressure or blood draws on the arm someone had surgery. Also listed were various things like avoiding gardening or getting manicures. However, new and updated research shows that these things do not directly cause lymphedema. Talk about confusing! It’s essential to explain why these precautions are listed on websites or handouts and why it is likely not the act of doing them that will cause lymphedema.
To summarize, each of these items listed is thought to have the potential to cause trauma to the skin, restrict blood flow, or increase the risk of infections. While taking blood pressure temporarily decreases blood flow, it has not been shown to change the lymphatic fluid flow. A blood draw, getting scratched, or a cut in the garden will cause a small opening in the skin. Getting a manicure or cutting cuticles can cause minor cuts or openings in the finger or nailbed. Although it’s very rare, anytime there is an opening in the skin; there is a risk for infection. An infection in the arm or chest on the side someone had treatment with may increase the risk of lymphedema.
So, when hearing or reading about these precautionary risks, it’s helpful to understand why they are being shared. Although they are not being found to cause lymphedema directly, they aim to keep the skin healthy and avoid infections to help lower the risk of lymphedema. Accidents do happen, though. If a cut or scratch does happen, cleaning it well and using an over-the-counter triple antibiotic cream can help lower any potential for infection. If a skin opening or wound is not healing or you think it may be infected, it’s best to contact your doctor for the next steps.
Ways to Lower the Risk of Lymphedema
With all the things that may increase someone’s risk of developing lymphedema, what about ways to lower one’s risk? There are three ways shown in research to lymphedema prevention. These include early detection, weight management, and exercise.
Early Detection
Early detection of lymphedema is critical because it’s one of the best chances for post-treatment prevention. Suppose lymphedema is caught early and treatment is started immediately. In that case, there is a greater chance of preventing the swelling from getting any worse; in some cases, it can reverse mild swelling. Early screenings at your hospital or clinic, using a measurement device, can help detect any signs of swelling and significantly lower the risk of chronic lymphedema.
It’s also important to know what signs and symptoms to look for yourself to reach out to your medical team for early treatment. Breast cancer-related lymphedema will only occur in the arm or chest on the side where the surgeon removed lymph nodes or radiated (the affected side). This will allow you to compare your affected side with the opposite arm and chest, which did not have lymph nodes removed nor radiated (the non-affected side).
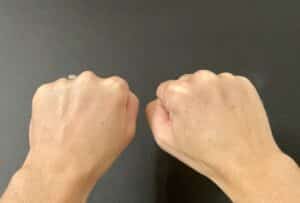
Make a fist with both hands and place them side-by-side. Look at your knuckles, tendons, and bones and see if there are changes or if you can no longer see these body landmarks on the affected side, but you can still see them on the non-affected side.
You will also want to stand in front of a mirror and look at the forearm, elbow, and breast or chest, comparing the two sides for any significant differences or changes.
You may notice that jewelry, bras, or clothes fit tighter on the affected side. Some may not see any swelling or change but may feel new aching or heaviness in the arm or breast. If you see or feel any other skin changes or have a cut that won’t heal, these may all also be signs of swelling or lymphedema, and it’s best to reach out to your medical team.
Weight Management
As discussed earlier, a higher BMI and obesity may increase one’s risk of lymphedema. Unlike the other risk factors like lymph node surgery and radiation, being overweight is something that can change. Medical reasons may make this challenging to do but working with your doctor or a dietician is a great place to start. It’s essential to stay as healthy as possible and maintain a healthy body weight for overall health, along with reducing the risk of lymphedema.
Exercise and Physical Activity
Exercise and physical activity play a role in a healthy lymphatic system and can also help lower the risk of lymphedema. The muscles in your body act as a pump for the lymphatic system. Muscles surround the lymphatic vessels. Activating the muscles can help stimulate the vessels, keep the lymphatic fluid moving in your body, and decrease the congestion of fluid. It’s important to start slow and low in weight and build up gradually to avoid overdoing it too soon. A physical therapist or certified lymphedema therapist in your area can help teach you safe and practical exercises.
Next Steps
Breast cancer-related lymphedema remains a side effect of cancer treatment that can be life-altering. The best thing to do is to communicate directly with your doctor and medical team about your risks and ways to be proactive in lowering the risk of developing lymphedema.
References:
DiSipio T, Rye S, Newman B, Hayes S. Incidence of unilateral arm lymphoedema after breast cancer: a systematic review and meta-analysis. Lancet Oncol. 2013 May;14(6):500-15. DOI: 10.1016/S1470-2045(13)70076-7. Epub 2013 Mar 27. PMID: 23540561.
Gillespie TC, Sayegh HE, Brunelle CL, Daniell KM, Taghian AG. Breast cancer-related lymphedema: risk factors, precautionary measures, and treatments. Gland Surg. 2018 Aug;7(4):379-403. DOI: 10.21037/gs.2017.11.04. PMID: 30175055; PMCID: PMC6107585.
Ferguson CM, Swaroop MN, Horick N, Skolny MN, Miller CL, Jammallo LS, Brunelle C, O’Toole JA, Salama L, Specht MC, Taghian AG. Impact of Ipsilateral Blood Draws, Injections, Blood Pressure Measurements, and Air Travel on the Risk of Lymphedema for Patients Treated for Breast Cancer. J Clin Oncol. 2016 Mar 1;34(7):691-8. doi: 10.1200/JCO.2015.61.5948. Epub 2015 Dec 7. PMID: 26644530; PMCID: PMC4872021.
Asdourian MS, Swaroop MN, Sayegh HE, Brunelle CL, Mina AI, Zheng H, Skolny MN, Taghian AG. Association Between Precautionary Behaviors and Breast Cancer-Related Lymphedema in Patients Undergoing Bilateral Surgery. J Clin Oncol. 2017 Dec 10;35(35):3934-3941. doi: 10.1200/JCO.2017.73.7494. Epub 2017 Oct 4. PMID: 28976793; PMCID: PMC5721227.
Naoum GE, Roberts S, Brunelle CL, Shui AM, Salama L, Daniell K, Gillespie T, Bucci L, Smith BL, Ho AY, Taghian AG. Quantifying the Impact of Axillary Surgery and Nodal Irradiation on Breast Cancer-Related Lymphedema and Local Tumor Control: Long-Term Results From a Prospective Screening Trial. J Clin Oncol. 2020 Oct 10;38(29):3430-3438. doi: 10.1200/JCO.20.00459. Epub 2020 Jul 30. PMID: 32730184; PMCID: PMC7527159.
Soran A, Ozmen T, McGuire KP, Diego EJ, McAuliffe PF, Bonaventura M, Ahrendt GM, DeGore L, Johnson R. The importance of detection of subclinical lymphedema for the prevention of breast cancer-related clinical lymphedema after axillary lymph node dissection; a prospective observational study. Lymphat Res Biol. 2014 Dec;12(4):289-94. DOI: 10.1089/lrb.2014.0035. PMID: 25495384.